Notes From the Mowed Down
I'm sitting here with a broken leg, and with nothing but time on my hands. It was little more than six weeks ago that a seventy-six-year-old psychiatrist from my hometown decided to drive home from work after dark, seemingly forgot to turn her lights on, pretended she was in a NASCAR race, and mowed me down as I was crossing a street on foot. She said she never saw me. It was mutual. I had been trying to get ice cream at a popular, local ice cream store, and had been crossing the street with my extended family in tow. Any one of us could have been hit, ranging from my 16-year-old niece to my ninety-three-year-old mom.
One moment I’m crossing the street and the next moment – after an ugly, surreal thud - I am sitting down in the road, holding my floppy right foot onto my leg so that the blood vessels would remain intact – some atavistic doctor instinct. This instinct just might have ended up saving my foot, by preserving the blood flow to already quite damaged tissues. I stayed preternaturally calm throughout, and remember saying to my wife, “Tell the kids I’m alive and it’s just my foot.” In the ambulance, they gave me two hundred micrograms of Fentanyl – enough for eight colonoscopies. It didn’t have the slightest effect on my pain. “Can I please have some more?” “Sorry – that’s the maximum.” They couldn’t give me anymore for fear I’d stop breathing.
I wasn’t aware that it was possible to feel this much pain. When pain is severe enough, it predominates over all other thoughts and feelings you may be having. I remember thinking, a little later, “Maybe I shouldn’t volunteer for Doctors Without Borders when I get older” – something I’ve always fantasized about. As someone once said, “Getting shot at wasn’t a big deal, it was actually getting shot that sucked.” I do not want to feel this level of pain ever again, no matter what.
***
Rushed to the hospital where I work, Man’s Greatest Hospital (M.G.H.), I suddenly found myself to be a center of attention. A flurry of activity was occurring that I can barely remember. I had entire conversations with doctors and nurses that were complete blanks as if I were an alcoholic in the midst of a blackout. In truth, they were giving me copious quantities of sedatives and opioids, which, along with the infinite level of pain, might have affected my memory. I don’t think I would have survived if they didn’t give me these meds.
During my evaluation, the trauma nurses unceremoniously snipped off my bathing suit while I had the incongruous and decontextualized thought, “Hey, that’s my favorite bathing suit”. No worry – I wouldn’t be swimming for a while. Maybe never at that point. I wouldn’t be walking or driving either for that matter. Earlier in the day, this bathing suit’s owner enjoyed a glorious day on the beach with my three adult children. This magical day was supposed to end with ice cream, not with them all witnessing me getting flattened by a distracted or impaired driver.
Having been through this ordeal, I feel as if I have special insight into what medieval tortures felt like for the people on the receiving end, or for what soldiers must go through when they step on a landmine.
***
Next, they geared up the complex and uncertain process of fixing my right leg. In medical terms, what I had was a comminuted (e.g., bone broken into pieces), open (i.e., bones poking out into the world where they certainly don’t belong – presenting a huge risk for infection), fracture of both my tibia and fibula - or an ‘open tib-fib fracture’. I have a blurry memory of signing a ‘consent’ for the first surgery, though what I was about to go through seemed like a foregone conclusion.
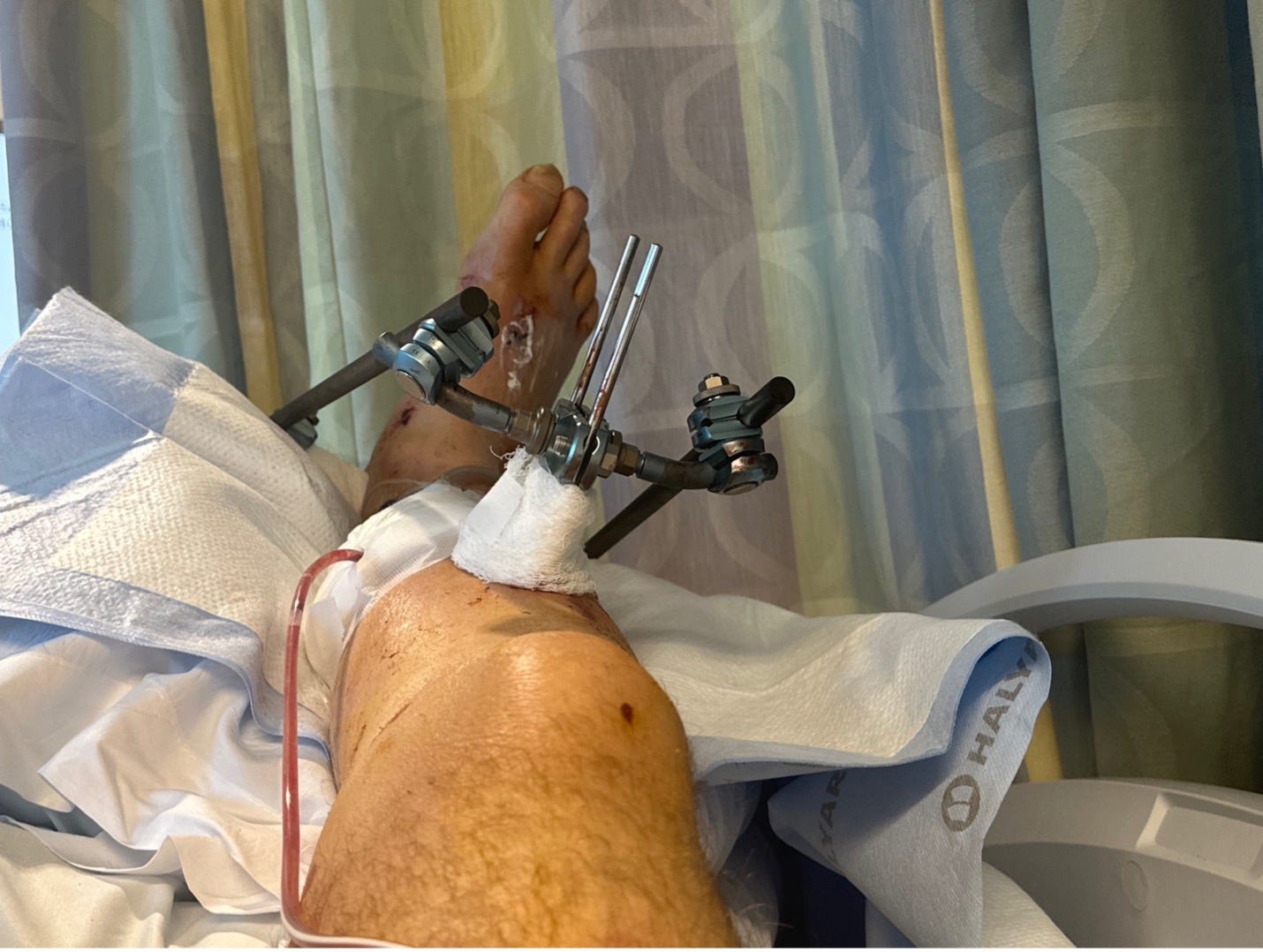
A standard surgical approach to address an open tib-fib fracture is the sequence of surgeries known as ORIF, or ‘Open Reduction, Internal Fixation’. During the first surgery, they anchored my bones and other tissues back into their proper location. To hold them in place, they attached a sort of external scaffolding to my leg by drilling screws into the bones of my heel and my shin. A picture is worth a thousand words.
Yes, it was just as painful as it looks! Even more so. The tiniest of movements resulted in an immediate, burning reminder that I had metal pins screwed into my bones in several different locations. Between the original injury and the surgery, I felt as if my leg had been dipped into a vat of hydrochloric acid. The pain went to eleven. Only opioids made this the least bit tolerable.
The words of the song, ‘Sister Morphine’ by the Rolling Stones, written about addiction, fully capture my growing desperation, as I was in excruciating pain, waiting each time for the nurse to come with the pain meds,
Here I lie in my hospital bed
Tell me, sister Morphine, when are you coming round again?
Oh, I don’t think I can wait that long
Oh you see that I’m not that strong
Not only was I waiting for Sister Morphine (or, technically, Uncle Oxy?), around the clock, I was awaiting my next surgery with trepidation.
***
Several days later, after a thermonuclear attack with very strong antibiotics on any potential residual microbes, to cleanse the tissue that should never have been open and exposed, I was due for the second surgery. This part is called “internal fixation”, the IF in ORIF, and it was hopefully the final, definitive surgery. Luckily, I was on a huge dose of ketamine, an interesting drug that I’ve written about for Harvard Health. I sorely needed the ketamine because, during this seemingly barbaric procedure, they injected a nail behind my right kneecap…ouch!... and thus inserted a rod into my leg, extending from my knee to my ankle, to hold my bones in close proximity. Once held together, the bones, especially the weight-bearing tibia, can ideally grow and heal together.
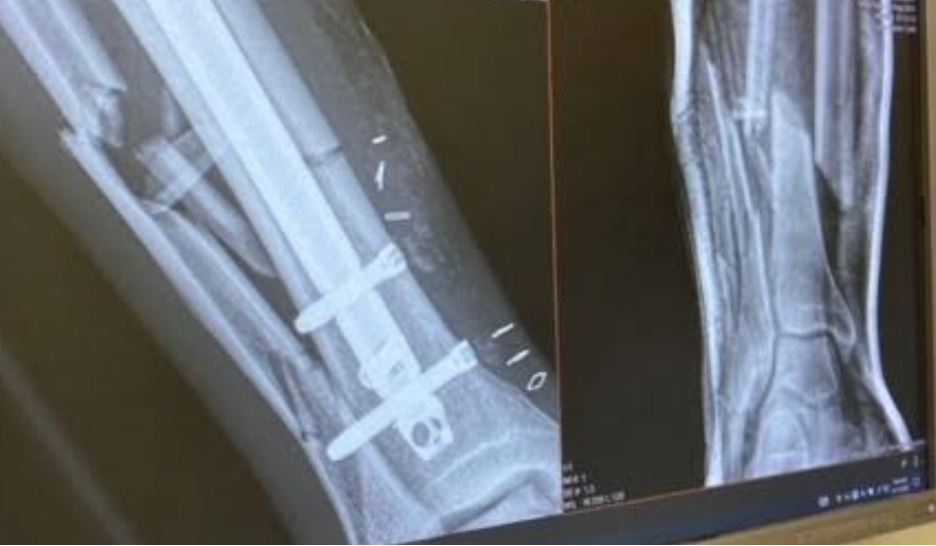
Here is a ‘before and after’ radiograph. On the right frame (before), just off the street, the bones are severely fractured, both the thicker tibia and the thinner fibula. You can see why my foot was flopping to the side. On the left of this X-ray, if you look, you can just see where the skin was punctured. On the left frame (after), several weeks out, I have the rod in place and my bones are starting to unite together. The most important bone is the thick one, a.k.a. the tibia, which bears most of the weight. This is just to the right of the rod and you can see it looking well-aligned.
Pain control: Cannabinoids and opioids
When in severe pain, such as after a traumatic accident like mine, or immediately after major surgery, opioids are required, period. Nothing else is strong enough, including cannabis, Tylenol or non-steroidals. It is inhumane and unethical to undertreat pain, even if you are worried that a certain percentage of people will ultimately get stuck on opioids (though, there are sensible ways to minimize the likelihood of this).
Unfortunately, as part of a highly misguided attempt to stem fentanyl overdosages, our government has been pressurizing doctors to not prescribe enough opioids. This is backfiring, as opioid overdoses haven’t dropped in response to this policy, but suicides have risen due to undertreated chronic pain. I discuss this in a piece in TIME Magazine. In short, as they deny people who are addicted, or people who are in chronic pain, sufficient access to opioids, patients buy these medicines on their own, and it is the illegal sale that results in so many people perishing from products tainted with fentanyl. If opioids were legal, available, and sensibly regulated, few would be dying from fentanyl.
On a visceral level, I wasn’t that excited to be taking opioids after my accident and my surgeries. This was due to my past addiction and the horrible associations I have with that miserable time in my life. This entire uphill battle against a near-lethal opioid addiction is recounted in my memoir, ‘Free Refills: A Doctor Confronts His Addiction.” Though, after this type of accident, and these painful surgeries, the pain was SO severe, I gladly accepted whatever opioids they would throw my way, much as a drowning person would accept a floatation device thrown to them in the water.
As a cannabis specialist, I was aware of research that cannabinoids can reduce the dose of opioids needed by co-working on overlapping receptors. For example, if you use 2.5 milligrams of oxycodone in an experimental situation, it doesn’t noticeably help with pain. If you use 2.5 milligrams of THC, the same thing: no pain relief. Yet, it has been shown that the 2.5 milligrams of oxycodone given with the 2.5 milligrams of THC can help control pain. There is a nonlinear, 1+1=3 phenomenon going on. I was able to leverage this knowledge to minimize both my pain and my opioid exposure. (People aren’t officially allowed to use cannabinoids in the hospital due the Federal illegality; this needs to change!)
I found that for every 2.5 milligrams of THC I was using I could go down on the opioids by about five milligrams. This made for much more coherent texts to friends and family and for a much more comfortable early recovery. Also, even though I’d been on opioids before, during prior surgeries, since my addiction, I know enough to attempt to minimize the dosage as able so as to not tempt fate. (I discuss pain control and the role cannabis plays in my new book, “Seeing Through the Smoke.”)
***
Wound care
A note on one of the underbellies of getting better: wound care. Wound care is a critical part of healing. I broke my leg, but the flesh wound was equally as complex to heal, requiring ongoing, sophisticated input from the experts in Plastic Surgery. In fact, they thought I didn’t have enough remaining healthy skin to cover up the wound and were strongly considering a skin flap – which is an utter nightmare involving a much more prolonged hospital stay, that I was able to avoid.
Wound care often requires dressing changes several times a day. It is not practical for the visiting nurses to come to your home anywhere near this frequently. So, ideally, a family member steps up and takes over the wound care. The two problems of this are one, it's gross, and two it can be quite complicated. One needs a family member or a friend who doesn't mind the grossness and can handle the complexity. Many families simply don't have this. As a consequence, they have much worse outcomes with their wounds.
Fortunately for me, my wife Liz, who is not medically trained (she is, however, a brilliant Data Engineer at one of the other Harvard Hospitals, though I’m not entirely sure what she actually does…) embraced my wound care and did an absolutely spectacular job. As I witnessed her meticulously addressing my complex wound, sometimes to the tune of several hours a day, I remembered that her father was a general surgeon. I could see the general surgeon genes operating within her – she would have been a phenomenal surgeon. Thanks to her competent and tender ministrations I was able to overcome two serious wound infections, avoid the dreaded skin flap surgery, and thus focus on healing my bones - which is the critical formula for success in an injury like this.
Conclusion
This entire accident has been an utter nightmare – literally the most difficult experience I have ever had to walk through (or, actually, limp through with a walker or, now, on crutches). For one, I thrive on exercise, and having to essentially sit still for several months has been utter torture. I feel like a puppy that has terrible owners and who, instead of getting tons of puppy-level exercise five times a day, is simply locked in its crate. It would take an entire other essay to list the things I had to cancel, the things I’ve missed out on, and how difficult it has been, at times, to maintain my mood above Dostoyevskian levels.
But there has been a massive bright side. The outpouring of love and support from friends, family members, and colleagues, is something I will remember and cherish for the rest of my life. It brought my family closer – nothing like all of us almost getting mowed down by a careless driver who was driving without looking at the road to bring you all together! I feel like I’ve grown, and many of my relationships have grown deeper.
I also have a more profound, if possible, love and respect for my partner Liz who has been with me every broken step of the way. Finally, I am grateful to still be alive – one step further and it would have been all over, as the driver would have mowed me down full-on, hitting much more than just my leg. I am not done yet.
P.S. This is me speaking, broken leg and all, at the recent Cannabis Science Conference in Rhode Island, with Cherissa Jackson and Brian Essenter, five weeks after the accident.





I wish you deep healing, and yes, your wife rocks!
Gwyllm
Thank you for everything! Wishing you a speedy recovery. -Edith & Sara